
Pakistan
Sindh Mobile Clinic Final Project Report
December 12, 2011
Dr. Rubina Mumtaz
Final Project Report for Sindhi Health Initiative

Background:
Following the devastating floods in Pakistan during the monsoon season of 2010, fundraising efforts were put into full swing by RMF. Dr Zeba Vanek, a neurologist and associate professor at UCLA, led one of our major initiatives. Dr Vanek had joined hands with RMF before to support relief efforts in Pakistan following the earthquake of October 2005. In addition, RMF’s association with the Sindhi Diaspora in the US resulted in another major fundraising effort to support the victims of the 2010 floods. Donors from both sides expressed their desire that the funds should be used to initiate an appropriate health intervention for the flood affected poor and vulnerable people of interior Sindh. For this aim, Real Medicine Foundation and the Sindhi Diaspora US jointly decided that the most appropriate intervention would be to address the health needs of the target populations in form of a Mobile Health Clinic that would travel long distances to remote villages which had been neglected by other relief efforts in the area.
Dr Geet Chainani, a physician and member of the Sindhi Diaspora in the US, volunteered to lead the proposed healthcare intervention. To serve as an implementing partner to the project, she founded a non-profit organization called ‘LifeBridge’ (LB) which was registered in both, the US and Pakistan. A MoU for a Mobile Health Unit Initiative was signed between Real Medicine Foundation and LifeBridge on January 5, 2011. District Dadu of Sindh was chosen as our field area of intervention. The steps of this unique intervention in the harsh setting of interior Sindh were:
Needs Assessment Survey:
RMF-LB Sindh Health Initiative began its operation in January 2011 by first networking extensively with the local health authorities and registering with the district health cluster coordinated by WHO and UNOCHA. Out of the four Tehsils in District Dadu, Taluka Johi was selected since it was the hardest hit by the floods due to its location between two major water sources, the MNV Drain and the FP Bund, both of which experienced an unprecedented deluge of flood water. Within Tehsil Johi, the local health department identified several union councils in need of health care intervention of which we randomly selected three for our needs assessment survey, namely UC Bahawalpur, UC Drighbala, and UC Pat Gul Mohammed. A local grass root NGO called Kachoo Foundation, based in Dadu City was taken on board for this exercise based on their knowledge of the local area, culture and colloquial.
The survey first assessed household based demographic evaluation of a randomly selected sample of villages using the WHO approved questionnaire. This was followed by a cross-sectional survey to assess the most current needs of incidences of water-borne diseases, general health ailments and the healthcare sought by the communities, given that several health partners were in operation on ground providing free primary health care. Our aim was not to duplicate services as well as have as high an impact as possible with the funding available to us. The results of the survey showed an alarming incidence of water-borne infectious diseases and malnutrition accompanied by a dismal level of all types of health care services accessible to the target population. The recommendation of the survey was to provide high quality primary healthcare and MNCH services in Union Council Bahawalpur targeting an estimated 20,000 people in this area. The reports of our needs assessments survey were shared with WHO and the local district level health department.
Field office:
In February 2011, a field office by our implementing partner, LifeBridge, was set up in Dadu City, equipped and staffed with the basic needs of an office. Care was taken to avoid extravagant expenditure of funds in line with our mission to utilize the majority of funds for actual services for the poor and vulnerable with a minimum usage for administrative purposes. A Toyota Hiace van was rented and its interior customized to make it suitable for outpatient services, with a special focus placed on the cultural gender issues of providing a safe and private environment for women to be examined by the Lady Health Worker (LHV). During the full tenure of the project, team members attended fortnightly meetings regularly and operated in close coordination with WHO Dadu, WHO Hyderabad and the district health department.
The AFYA Foundation of New York and the Sindhi Association of New Jersey had donated 2.5 tonnes of materials including clothes, blankets, water purification sachets and nutritional supplements to the Sindhi Diaspora US which were shipped to Karachi. Release of the container from the Karachi port and then onward transport by long-distance trucks was arranged to transport these donations to our Dadu office for distribution to the needy during our Mobile Health Unit (MHU) services.
Mapping Exercise and situational analysis of affected villages:
The basic principle of the MHU was to visit at least one village a day and request the community to come forward and avail the primary healthcare and MNHC services being offered. Villages were to be identified before the project was to begin; hence as a prerequisite for MHU operation, mapping of the villages of UC Bahawalpur was first conducted. The mapping exercise identified the 16 most affected villages for whom a detailed situational analysis was carried out. These villages had been wrecked beyond recognition and residents had set up makeshift homes. Large stagnant pools of water were still present, creating a source of mosquito-borne diseases. The main water body was contaminated making available drinking water toxic. The situation analysis stage was completed by March and the results were shared with WHO and the local district level health department.
MHU Primary healthcare service operation:
The situation analysis stage was unfortunately not followed by immediate MHU operations due to an unexpected change in donor commitment causing a sudden but temporary pause in the work for the month of March. The funds gap was satisfactorily addressed within a short period. On getting back onto the field, a new issue of lack of skilled medical staff willing to rough it out in the field in this hot, stifling summer arose. This unavailability could be attributed to the fact that most of the other health partner organizations working in Dadu had chosen to set up static clinics in urban towns and cities making it easy for medical personnel to find quality employment within the comfort of their hometowns. It took us two weeks to find qualified and willing medical workers and the MHU began operations in mid April 2011 and ended in July 2011. During the tenure of our MHU from January-July 2011, RMF-LB was the only organization providing healthcare for the entire Union Council Bahawalpur since other organizations had wrapped up their activities and moved on to rehabilitation activities despite the fact that the communities had no healthcare services in place.
The MHU services operation protocols were as follows. It offered services from 9.00 am to 4.00 pm, six days a week. On a daily basis, a pre-determined amount of medicine and surgical supplies were procured from the office stocks and the team composed of the Medical Doctor, the Lady Health Visitor, the Dispenser, the Field Supervisor and an Armed Guard set off to the pre-designated village of the day. The presence of a fully armed security guard was essential for the security and safety of the RMF-LB team in lieu of the increased lawlessness of interior Sindh post floods. The doctor and the LHV saw patients separately, with the latter exclusively for women and infants. A special focus was on identification of malnutrition cases. The dispenser disbursed medicine and nutritional supplements according to the prescriptions given by the two healthcare providers. The field supervisor’s duties were to liaise with village elders and under their guidance, make either house-to-house visits or hold community-centered sessions for relaying of basic hygiene and health awareness messages, with a special focus on healthy drinking water. These house-to-house visits were accompanied with disbursement of donated goods and water purification sachets.
Most of the diseases diagnosed and treated by the doctor were a result of the contaminated water sources, increased temperatures and a general lack of sanitation and hygiene. They included:
- Acute Respiratory Tract Infections
- Acute Watery and/or Bloody Diarrhea
- Dyspepsia and abdominal pains
- Scabies
- General body aches and weaknesses
- Malaria
In addition, the Lady Health Visitor saw cases of menstrual irregularities and other gynecological/ obstetrics problems.
Result of Mobile Health Unit intervention:
Demographics
A total of 73 affected villages were visited. The sizes of villages varied but an average village was composed of approximately 30 households averaging a population of 200 persons. Smaller villages were visited once but average or large villages were visited at least twice to ensure access to as many persons as possible in need. Hence our MHU made available high quality primary and MNCH healthcare to an estimated population of 16,000 people which is about 80% of the population of Union Council Bahawalpur (20,000 persons). The villages visited according to the months were:
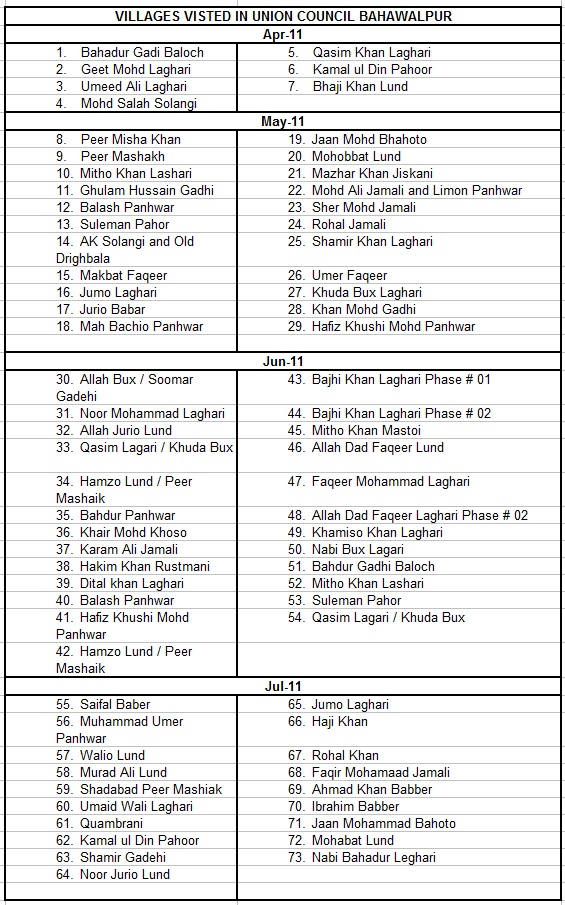
Morbidity statistics:
Monthly DEWS reports were made and shared with the WHO and local health authorities. During our MHU services on the ground in UC Bahawalpur in Dadu, a total of 5,675 men, women and children were attended to and treated for target illnesses. Of these, 1,955 (34.5%) were children. Of the adult population, the gender distribution was 1,561 (41.9%) women and 2,159 (58.1%) men.

The patients presented with the following health problems:
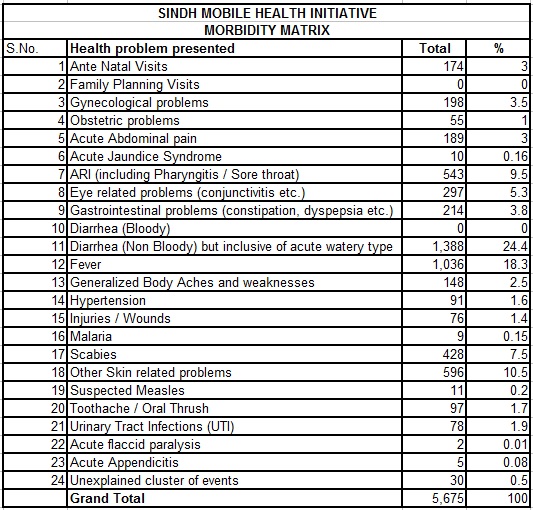
The most commonly presented illness was non-bloody diarrhea (1,388 – 24.4%) out of which 18 cases were of acute watery diarrhea which were registered and treated accordingly. Luckily no case of bloody diarrhea was encountered. The second most common illness was unexplained fever at 18.3% closely followed by skin-related problems at 18%. Nearly half of the dermatology issues were scabies that can be attributed to the unhygienic living conditions that these poor people are forced to adopt given that they had lost their homes and all accompanying means of comfortable and quality day-to-day living in the devastating floods.
Other illnesses presented were respiratory issues at 9.5% inclusive of acute respiratory tract infections as well as acute pharyngeal infections and common sore throats. Gynecological/obstetric problems constituted 7.5% of the illnesses followed by eye-related issues and gastrointestinal problems at 5.3% and 3.8% respectively. A wide range of other illness made up for the rest of 13.2% of the health problems presented at our MHU. A graphical representation is as follows:
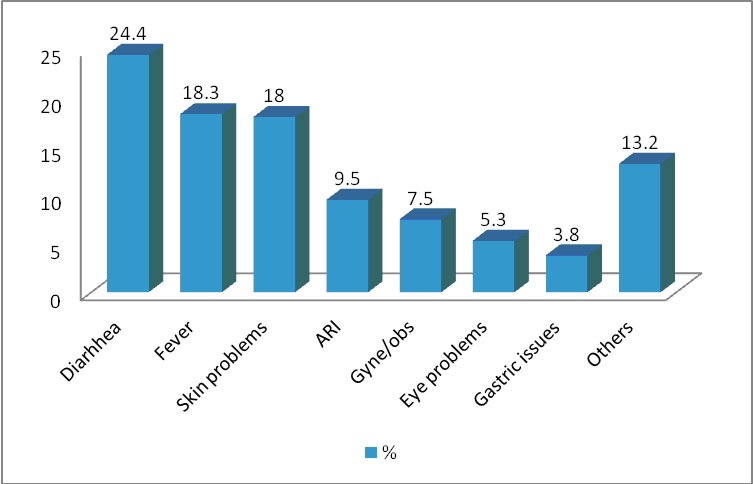
Mother and Child Health:
Gynecological and obstetric issues constituted a significant part of the health issues presented by 427 out of 1,561 women. Of these, 174 women came for ante-natal check-ups, a first time for the majority of these expectant mothers. All of them were visibly anemic and most suffered from mild to moderate malnutrition. All these women were given nutritional supplements. Interestingly enough, not a single woman came forward to ask about family planning methods although the issue was raised with nearly all the women of child-bearing age that visited the LHV. The qualitative feedback given by the LHV was that a majority of the women relied upon traditional methods of contraception and when these methods failed, they resigned to their fate and embraced their pregnancies with the belief that this child/life was meant to be borne – a directive from God.
The remaining 253 women presenting with OB/Gyn related issues were treated by the LHV. Two women were referred to the Dadu THQ hospital, and transport was provided for by the MHU.
During the house-to-house visits, 226 lactating mothers were identified and the majority was found to be suffering from mild malnutrition. The women were given nutritional supplements. In total 400 PLWs (pregnant and lactating women) were given nutritional supplements during our MHU services in the UC Bahawalpur.
Children under the age of 5 years were particularly targeted by our health team to evaluate them for malnutrition. In total 420 children under five were diagnosed with mild to moderate malnutrition and were given pediatric nutritional supplements in form of drinks. Unfortunately for many this was a one-time activity which would have no impact on their general health. There is a dire need to maintain these nutritional supplements on a sustainable level.
Children constituted a significant portion of the diarrhea cases presented to both the doctor and the women. Therefore 5,000 liters of ORS were distributed to children as a measure to address the increased incidence of diarrhea during our MHU services on ground.
Health awareness sessions and distribution of donations:
House-to house visits were conducted by the field supervisor in each village. For larger villages where this activity would take more than a day, the village elders were consulted and requested to inform the villagers to come to a central point in the village to learn about basic hygiene and health issues that can be addressed by having the awareness and knowledge of simple preventive measures. The main focus was on clean water which was major obstacle in the flood affected villages. Our situational analysis had shown us that most of the villages’ main drinking water body was contaminated with heavy deposits of mud, debris and on many occasions, dead animals. Naturally the most commonly encountered health problem was diarrhea as the villagers had no option but to drink the dirty water to combat the extreme temperatures in the desert landscape. Our awareness sessions were accompanied with distribution of water purification sachets. Distribution was carried out on a household basis which according to the Survey of Pakistan is 7.3 members per household. Hence, approximately 4,000 people received clean water for every month we were on ground.
The health awareness sessions were often accompanied by distribution of the donated items by AFYA Foundation. In total 387 families received blankets while 800 adults and 800 children received 2 new outfits each.
Notable project challenges and obstacles:
Interior Sindh is a particularly difficult area to work in for a variety of reasons. The main notable challenges our project faced were:
• Tough environmental conditions: Geographically, Sindh is bounded by the Thar Desert to the east, the Kirthar Mountains to the west, and the Arabian Sea in the south. In the centre is a fertile plain around the Indus River, the source of the flood water. Hence it lies in a tropical to subtropical region where it is very hot in the summer with temperatures frequently rising above 45oC (115o F). The thermal equator passes through upper Sindh, where the air is generally very dry. Sandstorms are a common occurrence, sometimes several times a day often forcing the MHU to park on the side till the storms subsided.
• Damaged roads: Most of the roads, which were originally not of the best quality, were destroyed by the flood waters. So huge pot holes slowed the speed of the MHU. On several occasions, the roads were completely broken down to reveal deep ridges and gorges forcing the MHU to find a circuitous route to the destination. Delays in travel meant less time to open clinic operations since it was imperative that the team reach back to the field office before dark for security reasons.
• Low levels of literacy: Low levels of literacy; particularly in English fluency was a major hurdle in our report writing. This can be attributed to the fact that most educated people of this rural area grabbed the first opportunity to move to the urban areas for better lives and prospects. Willingness to work in the backwaters of Dadu and particularly at grass root level right into the villages meant that we got very few qualified and experienced applicants for our staff positions in both the administrative section as well as in the medical team. Looking for the right personnel created an unnecessary delay in launching the field healthcare services of our project, a precious loss of time in which we could have reached a lot of poor and vulnerable people.
An additional factor that was highlighted during our time on ground was the low motivation of the staff for field work. Absenteeism was a frequent occurrence and intense team energizing with pep talks were the call of the day.
• Funding availability: Lack of funding meant that the project had to close up within 6 months at a time when it was at its peak. The MHU had established a reputation in the area and as the word of our high quality healthcare services spread, the field office was getting requests to visit additional villages in the other union councils. Unfortunately funding became a major obstacle that prevented us from continuing the good work.